 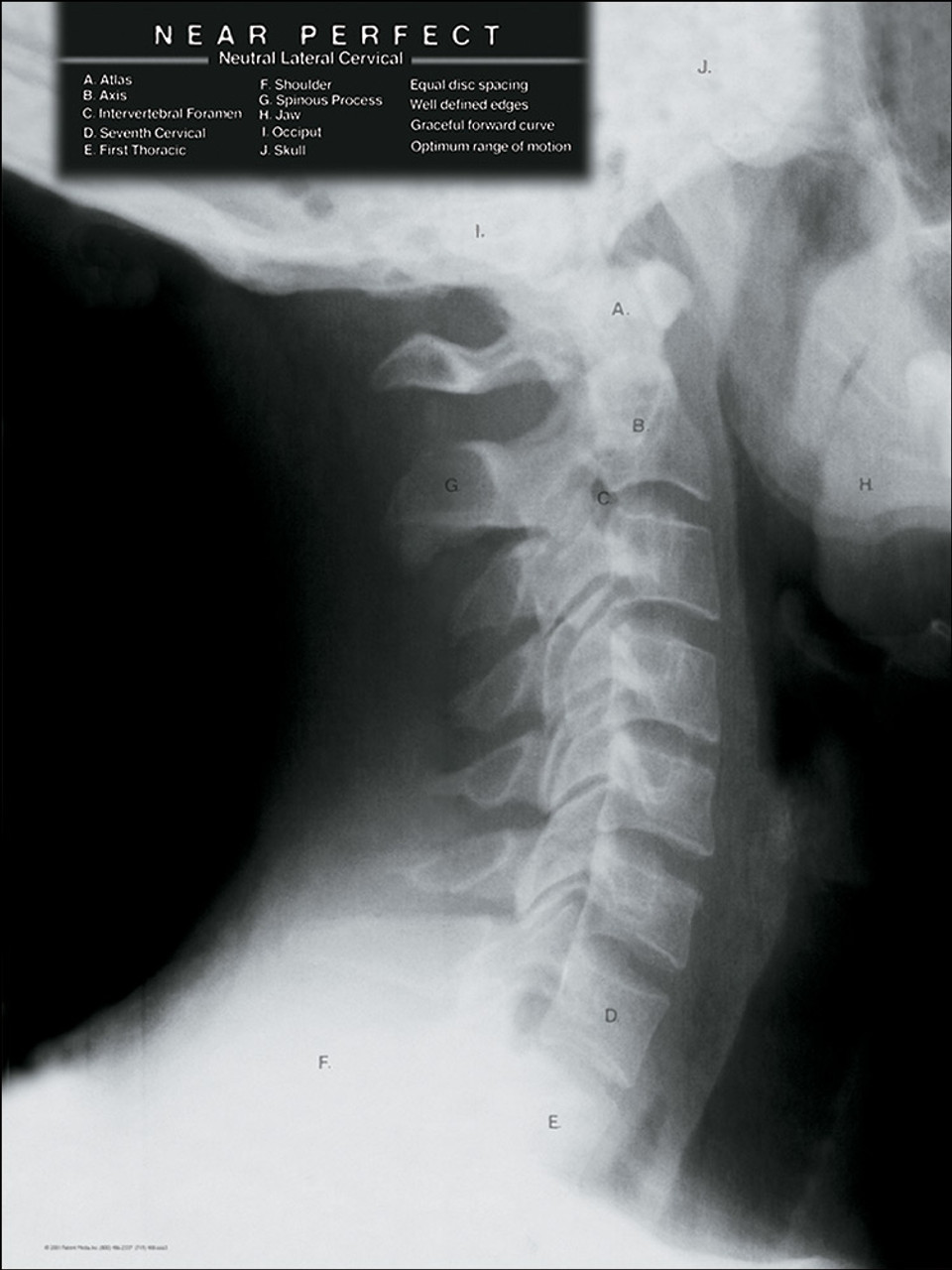
The list in Table 3-1 can guide you to the relevant figure, where diagnostic features are discussed in detail. The figures in the chapter span a range of important spinal pathology, moving from cephalad to caudad. The figure captions are designed to allow the figures to stand alone, so we spend relatively little time discussing specific fracture patterns in the text. Don’t be daunted by the number of figures in this chapter-we explore injuries and nontraumatic spinal pathology in many imaging planes and in multiple modalities to maximize your three-dimensional understanding. We correlate CT findings with x-ray when possible, and we demonstrate associated soft-tissue abnormalities identified on magnetic resonance imaging (MRI). Our discussion of all spinal regions starts with interpretation of images, with a focus on computed tomography (CT) scan. Although differences exist, many common themes are shared in both the selection and the interpretation of diagnostic studies for all regions of the spine. Smooth and continuous and that C2 does not appear "fat" (i.e.In this chapter, we discuss imaging of the cervical, thoracic, and lumbar spine. Make sure the basion-dens space is Make sure the atlantodens interval (ADI or pre-dental space) is Check that the intervertebral spaces are uniform at each level.Surface of the occipital and sphenoid bones) Clivus should be pointing toward the odontoid (the clivus lies at the base of the skull is made from the.Inspect each vertebral body, pedicle, lamina and spinous process from C1 - C7 Check the posterior vertebral line (posterior longitudinal ligament line).Check the anterior vertebral line (anterior longitudinal ligament line).Evaluate the orientation of the epiglottis, hyoid bone, tracheal shadow and check for any foreign bodies.Vertebral body) and < 22 mm in front of C6 (or no more than width of C6 Tissue is < 7 mm in thickness in front of C2 (or < 50% of the width of C2 Make sure you can see all 7 cervical spinous process.The clinician should establish a process or order they follow each time. To the tip of the dens (or odontoid process). The dorsal surface of the clivus and is used to measure the distance of space This is a line drawn from the caudal extension of The tip of the dens should lie less than 4.5 cm above this line. Draw a line from the posterior edge of the hard palate to the caudal end of the occipital curve. Opisthion (posterior aspect of the foramen magnum) cannot be identified on a To recognize the presence of basilar invagination (a craniocervical junctionĪbnormality where the tip of the dens project up into the foramen magnum). If the tip of the dens extends > 3 mm above this line then it helps.The odontoid tip extends above this line. Posterior surface of the hard palate to the tip of the opisthion (posteriorĪspect of the foramen magnum) and is used to measure the distance of how much (normal CT values for men is > 23.7 mm and for women is > 24.2 mm) can be used instead. Tip of the dens is eroded then the Redlund-Johnell and modified Ranawat methods The dens (or odontoid process) should be ~5 mm below this line. Lateral radiograph of the skull or on a sagittal cut from a CT or MRI scan thatĬonnects the posterior and anterior aspects of the foramen magnum. Note: Scroll over or tap on the image to see labels & lines 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
